Electrooculography (EOG) is a visual electrophysiology test that measures the resting potential of the retinal pigmented epithelium (RPE) in response to darkness and light. EOG responses are abnormal in conditions that affect the RPE or disrupt dark adaptation. Patients with Best’s disease and will likely have affected EOGs.
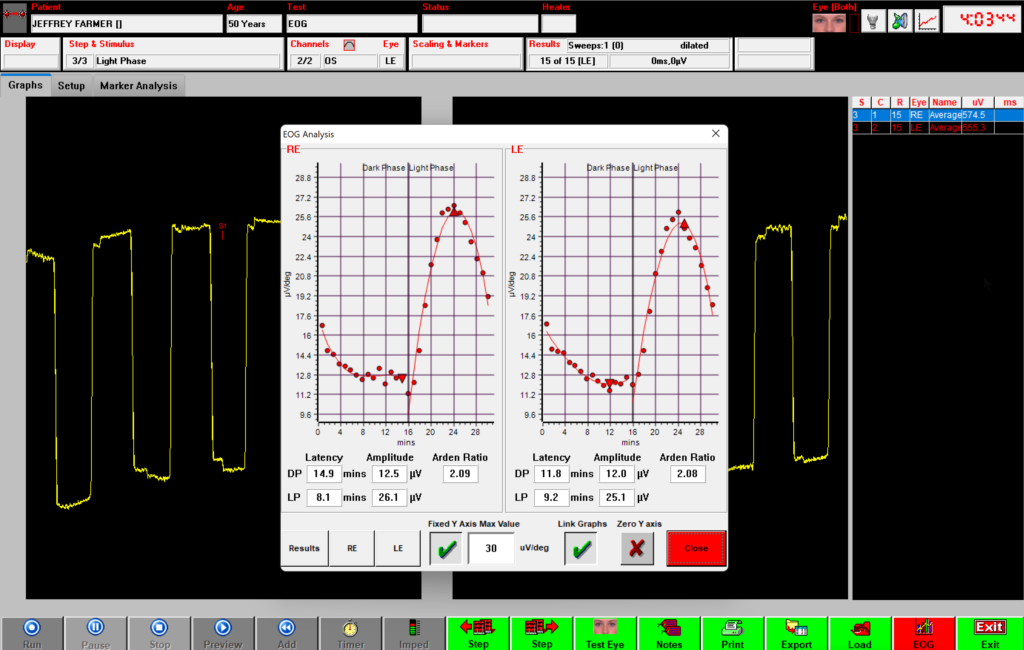
Perform an EOG test
The EOG test primarily measures changes in the voltage of the RPE under dark and light conditions. To accomplish this, patients sit with their heads in the ColorDome®. Electrodes are placed at the nasal and temporal canthi. Room lights are turned off to begin the test. The patient dark adapts while following a single oscillating LED light, making smooth 30-degree horizontal saccades with their eyes. After 15 minutes, background lights turn on and the test continues in the light.
RPE voltage potential
The EOG test measures the electrical potential difference between its front (anterior) and back (posterior) of the eye, referred to as the standing potential of the eye. This standing potential indirectly measures the transepithelial potential (TEP) of the retinal pigment epithelium (RPE). The TEP results from the difference in membrane potential between the RPE’s basolateral and apical membranes, which are electrically isolated by the tight junctions of the RPE. Alterations in resistance or membrane potentials between these membranes change the TEP amplitude, thereby affecting the recorded standing potential of the eye. Additionally, changes in ambient light can induce variations in the standing potential through retinal adaptation.
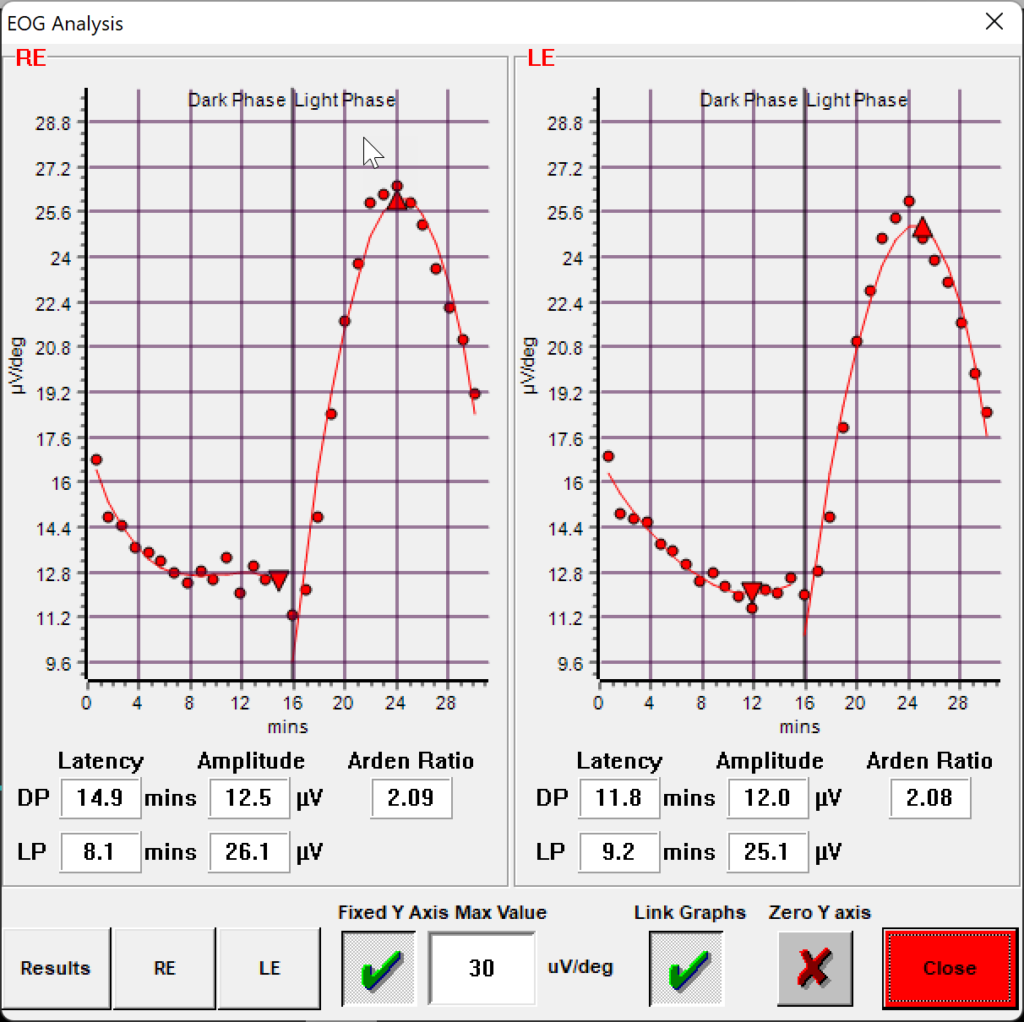
Calculate the Arden ratio
The final output of an EOG test is a calculation of the Arden ratio. Calculate the Arden ratio by dividing the highest light phase amplitude (light peak) by the lowest dark phase amplitude (dark trough). Normal Arden ratios typically range between 1.7 to 4.3. Ratios lower than 1.7 may indicate abnormalities in the RPE and can be associated with Best’s disease or other diseases affecting the RPE and outer retina.
References
Constable, P.A., Bach, M., Frishman, L.J. et al. ISCEV Standard for clinical electro-oculography (2017 update). Doc Ophthalmol 134, 1–9 (2017). https://doi.org/10.1007/s10633-017-9573-2
